Microsurgical Testicular sperm Extraction (Micro-TESE) for Azoospermia
Men with non-obstructive azoospermia have a problem with sperm production in the testicles – there is either zero sperm cells being produced or only a tiny amount of sperm which is insufficient and not picked up when analyzing the ejaculate.
Some of the causes of non-obstructive azoospermia include:
- Infections: Mumps that spreads to the testicles
- Genetic: Sex chromosome abnormalities, Klinefelter syndrome
- Undescended testicles
- Chemotherapy for cancer treatment
- Developmental abnormalities of the testicles
Until recently there was very little hope of fertility for men with non-obstructive azoospermia and it was only in very rare cases that testicular sperm production could be recovered. However, in the last 20 years, major breakthroughs lead to the discovery that up to 60% of men with non-obstructive azoospermia actually have sperm present in their testicles and that this sperm can be obtained microsurgically and used for assisted fertility procedures (ART / IVF / ICSI).
Subsequently, the technique of Microdissection Testicular Sperm Extraction (micro-TESE) was developed for obtaining sperm cells from these men, and today many men with non-obstructive azoospermia are able to have children of their own.
The Micro-TESE Procedure
Micro-TESE or Microdissection Testicular Sperm Extraction was first described in 1999 as an effective method of obtaining sperm from men who were considered infertile due to non-obstructive azoospermia.
Before this, men with non-obstructive azoospermia were considered completely infertile with no hope of fathering their own children. The only options available to them were adoption or the use of donor sperm.
The Micro-TESE procedure is performed in a fully equipped operating room as day case surgery (no overnight stay required). You need to be nil by mouth for at least 6 hours prior to the operation. Because of the fact that the entire operation is performed with the surgical microscope, my patients need to remain absolutely still for the duration of the surgery – for this reason general anesthesia (patient completely asleep) is used for all cases.
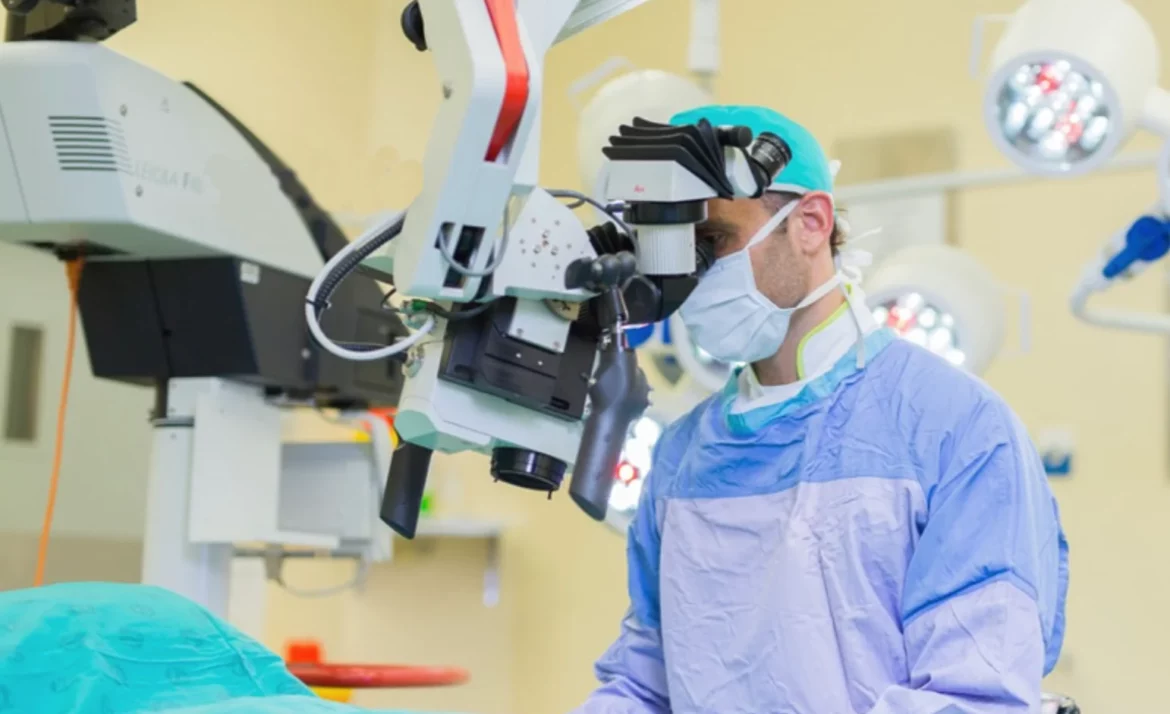
Prof Zarrabi uses a surgical microscope which provides up to 40X magnification
Micro-TESE Surgery Step-by-Step:
An incision of about 2,5cm long is made into the scrotal skin, on the midline of the scrotum – this approach has the following advantages:
- Access to both testicles through a single incision
- Good cosmetic result post-operatively
- Minimal pain
One of the testicles is then delivered through the skin incision. The decision on which testicle (left or right side) to start with, is based on careful physical examination by myself – studies have clearly shown that if one of the testicles is larger and firmer than the other, the larger testicle has a better chance of containing sperm.
Once the testicle has been brought into view, the surgical microscope is placed over the operating field and used for the rest of the operation. A surgical microscope gives up to 40X magnification and is absolutely essential when performing Micro-TESE.
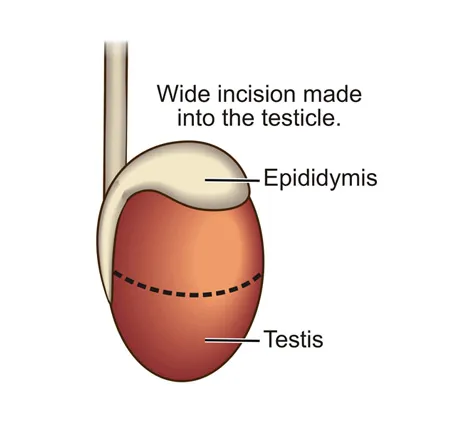
A wide incision is now made into the layer of tissue that surrounds the inside of the testicle (testicular capsule). With the help of the surgical microscope, even the tiniest blood vessels can be identified – care is taken to preserve these fine blood vessels that run underneath the capsule of the testicle because injury to these structures can lead to complications post-operatively.
A wide incision is made through the testicular capsule
Microsurgical instruments are used to search the inside of the testicle for tubes that contain sperm
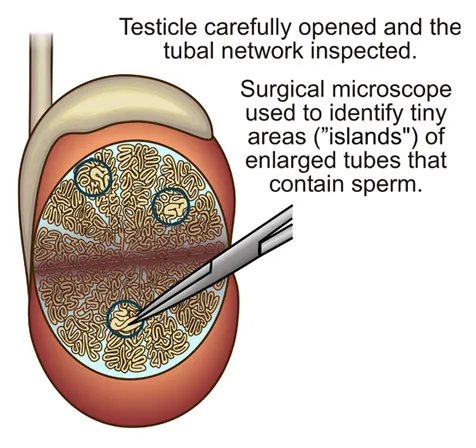
The testicle is then opened up and the inside inspected. Sperm production in the testicle takes place in a network of very thin tubes (seminiferous tubules) and under conditions of normal sperm production, these tubes are relatively large (dilated). Patients with non-obstructive azoospermia have thin, collapsed tubes because no or very little sperm production is taking place.
In patients with non-obstructive azoospermia and zero sperm in the ejaculate, up to 60% will still have small areas of sperm production inside their testicles. The surgical microscope is now used on high magnification to find these tiny areas where the tubes are dilated and sperm is likely being produced.
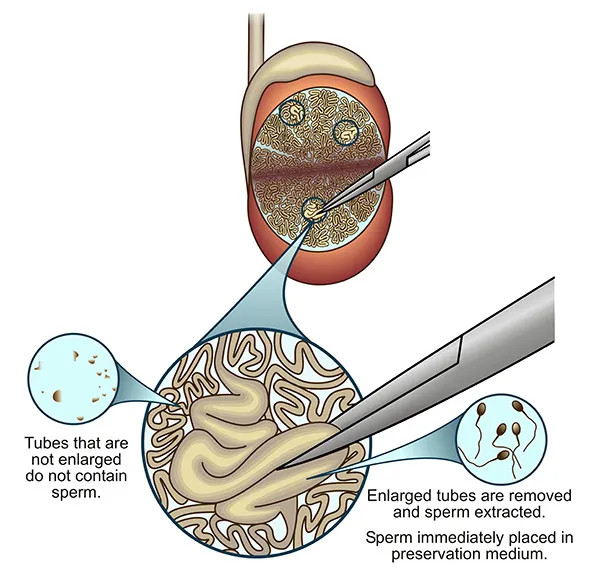
Enlarged (dilated) tubes are identified, removed, and evaluated in theatre using a light microscope that provides 400X magnification. Several areas of dilated tubes may be sampled until adequate sperm is identified, which is then processed in theatre and cryo-preserved (freeze-stored) for later use in Assisted Fertility procedures (ART / ICSI).
Enlarged tubes are carefully removed and thoroughly inspected for the presence of sperm
After meticulous inspection of all the testicular tissue under the surgical microscope, and biopsy of all areas likely to harbor sperm, the testicle is carefully stitched closed. A very fine suture is used and care is taken to not leave any areas of bleeding inside the testicle. The testicle is then placed back into its normal position inside the scrotum and the same procedure repeated on the other testicle.
After completion of the operation, the scrotal skin is closed. For this, I use a stitch that dissolves after about 3-5 weeks. A tight dressing (“jockstrap”) is placed on the scrotum to prevent bleeding. You will be able to go home later that same day and will receive a prescription for pain medication. You will not be allowed to drive a car for the first 24 hours after the procedure, so be sure to have someone available to take you home from the surgical facility.
What Happens with the Extracted Tissue?
All of the testicular tissue which was biopsied is sent to our state-of-the-art fertility laboratory. Here, our dedicated team of embryologists and laboratory staff will now spend a couple of hours going through all of the tissue to find and extract the sperm. Only after this part of the process has been completed, will we know whether your operation had been successful (ie if there was indeed useable sperm present). All of the sperm which is obtained is then freeze-stored (cryo-preserved) at the fertility laboratory. The cryo-preserved sperm can at any time be couriered to the Fertility Centre of your choice (locally or internationally) for use in assisted fertility procedures (ART / ICSI)
After the Operation
Recovery: Do’s and Don’ts
- Better to take it easy for the first day or two. Go directly home after the operation and rest: elevate your feet. Plan to limit the time on your feet as much as possible for the first few days.
- The local anaesthetic will wear off within about 3-6 hours after the operation and you will be provided with a prescription for pain medication when you leave the clinic.
- Locally applied ice packs in the first 24 hours as well as a tight scrotal support garment (will be provided to you) for a few days, are very effective in preventing post-operative pain and swelling.
- You will usually be given sick leave for 7 days but you may return to work earlier if you feel up to it and provided that your occupation does not involve physical exertion (lifting of heavy objects, walking long distances) or standing for long periods.
- You should avoid heavy physical activity for approximately 2 weeks and may resume sexual activity 1 week after the procedure.
Complications
Although micro-TESE is a minor procedure, any surgery on the human body carries with it the risk of possible complications. Fortunately, complications after micro-TESE are relatively uncommon. Even if a complication does occur, it is usually more bothersome than serious and are mostly treated conservatively (ie no surgical intervention required).
Complications that may arise include:
There is virtually no bleeding during the operation, but bleeding on the inside of the scrotum (wound hematoma) causing swelling and bruising may take place in the days following your surgery. Should this occur, the treatment will usually involve a course of antibiotics and anti-inflammatory medication, ice packs, plenty of rest and also a tight-fitting scrotal support garment. Most of these hematomas will resolve on their own and there will be no long-term effects. It is important that you take it easy for the first few days after your surgery in order to further reduce the risk of a wound hematoma.
There is no benefit in routinely taking a full course of oral antibiotics after your operation – in fact, this practice increases the resistance of germs to antibiotics. Superficial wound infections may rarely occur after micro-TESE, and will usually be managed with a course of oral antibiotics and daily cleaning of the wound with a saltwater solution.
During the micro-TESE procedure, the entire testicle is opened and surgery is performed deep inside the testicular tissue. The surgeon needs to be extremely careful to ensure that the fine blood vessels that run inside the testicle are preserved. For this reason, the use of a high-quality surgical microscope and precision microsurgical instruments is essential. Damage to the blood vessels inside the testicle may lead to testicular compromise and even loss of the testicle in the days after the operation.
Another complication of blood vessel damage is post-operative bleeding inside the testicle – this will cause an increase in pressure in the testicle, which may also compromise the function and viability of the testis.
Proper microsurgical technique and the use of the appropriate equipment are the best ways to ensure a safe micro-TESE procedure and prevent complications
Success Rates
Microdissection Testicular Sperm Extraction (micro-TESE) is the preferred method of obtaining sperm cells from men with non-obstructive azoospermia so that they can be biological fathers.
For every patient, the success rate of micro-TESE (ie obtaining useable sperm from the testicles) is to some extent dependent on the specific reason for him having non-obstructive azoospermia.
The table below summarizes data from international studies on the most common causes of non-obstructive azoospermia and indicates the success rate of the micro-TESE procedure in each of these conditions:
| Cause of Non-Obstructive Azoospermia | Success Rate (Obtaining useable sperm) |
|---|---|
| Chromosome abnormalities | 67% |
| Undescended testicles | 62% |
| Klinefelter Syndrome | 61% |
| Chemotherapy | 42% |
Note: It is important to remember that a successful micro-TESE procedure does not guarantee pregnancy. The role of micro-TESE is to obtain sperm cells from the testicles of men who have no sperm in their ejaculate. After successful extraction of the sperms, they are freeze-stored (cryo-preserved) in a fertility laboratory. The sperm can then be couriered to the Fertility Centre of the patient’s choice (nationally or internationally) for use in assisted fertility procedures (ART / ICSI).
